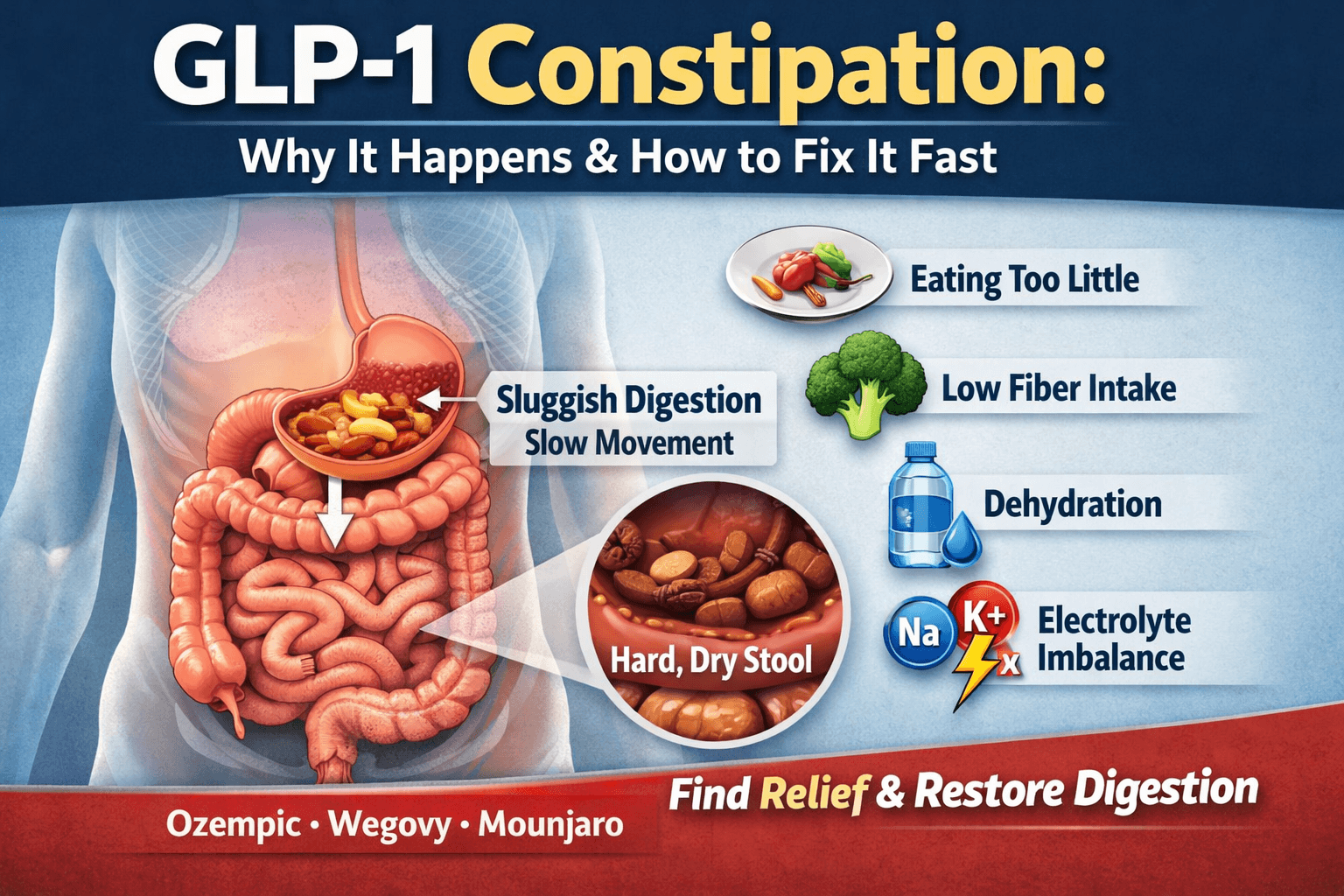
If you’re taking Ozempic, Wegovy, or Mounjaro and suddenly struggling to go to the bathroom, you’re not imagining it — and you’re definitely not alone.
Constipation is one of the most common and frustrating side effects of GLP-1 medications, and for many people, it becomes a daily problem that affects comfort, energy, and even weight loss progress.This is a well-documented response to how these medications work inside the body.
GLP-1 receptor agonists change the way the digestive system functions. They slow the rate at which food moves through the stomach and intestines. While this is part of what makes them effective for weight management, it also means the digestive process takes longer — and bowel movements can become less frequent.
The good news is that GLP-1 constipation is usually manageable. When the right nutrition and hydration strategies are in place, most people see significant improvement. This article explains exactly why constipation happens, what is driving it, and what you can do to relieve it safely.
We will cover the following causes in detail: slowed digestive motility, reduced food intake, low fiber consumption, dehydration, electrolyte imbalance, and physical inactivity.
How GLP-1 Medications Affect Digestion
GLP-1 stands for glucagon-like peptide-1. It is a hormone the body naturally produces in response to eating. GLP-1 receptor agonists are medications that mimic this hormone’s effects — but at a much stronger and longer-lasting level than what the body produces on its own.
These medications work through several mechanisms:
- Slowed gastric emptying — food stays in the stomach longer before moving to the intestines.
- Appetite suppression — strong signals of fullness reduce the desire to eat.
- Reduced food intake — overall calorie and volume consumption drops significantly.
- Changes in digestion speed — the entire digestive process moves more slowly.
These effects are why medications like Ozempic (semaglutide), Wegovy (semaglutide at a higher dose), and Mounjaro (tirzepatide) are effective at reducing appetite and supporting weight loss. However, the same mechanisms that help with weight management are also responsible for the digestive side effects many users experience — particularly constipation.
When food moves through the digestive system more slowly, the colon absorbs more water from the stool. This leads to harder, drier stools that are more difficult to pass. Combined with eating less food overall, the result is often significantly reduced bowel movement frequency.
The digestive slowdown caused by GLP-1 medications is well documented in clinical research. These medications alter gastric emptying and intestinal movement, which directly impacts how quickly food and waste move through the body. This is why many of the known GLP-1 medication side effects are linked to digestion, including constipation.
Why Constipation Happens on GLP-1
Constipation on GLP-1 is rarely caused by one factor alone. In most cases, it is the result of several things happening at the same time. Understanding each contributing cause is the first step to addressing the problem effectively.
The most common causes include:
- Slower digestive motility caused by the medication itself
- Dramatically reduced food intake leading to less digestive stimulation
- Low fiber intake from eating less food overall
- Dehydration from reduced appetite and thirst signals
- Electrolyte imbalance affecting gut muscle contractions
- Reduced physical activity lowering natural digestive stimulation
Cause 1: Slower Digestive Motility
GLP-1 medications are specifically designed to slow gastric emptying — the rate at which food leaves the stomach and enters the small intestine. This slowing effect is one of the key reasons people feel full for much longer after eating smaller amounts of food.
However, the slowdown does not stop in the stomach. When gastric emptying is delayed, the entire gastrointestinal tract tends to move more slowly. This means food and waste take longer to travel through the small intestine and colon. The longer stool sits in the colon, the more water is extracted from it — resulting in harder, dryer stools that are more difficult to pass.
This is the foundational cause of GLP-1 constipation. Even with good hydration and fiber intake, the reduced transit speed can still contribute to less frequent bowel movements.
Cause 2: Eating Much Less Food
Many people using GLP-1 medications experience a dramatic reduction in appetite. Some go from eating three full meals per day to barely finishing one. This level of appetite suppression can feel like progress — and in some ways it is — but it creates a real problem for the digestive system.
The digestive system depends on food volume to function properly. Every time food enters the stomach, the digestive tract is stimulated to contract and move contents forward. When food intake drops significantly, there is less material to stimulate those contractions. Less movement means less frequent bowel movements.
Eating too little is a common and underappreciated problem for GLP-1 users. When food intake drops too far, the body may not be getting enough nutrients to support muscle preservation or metabolic function — and it can worsen constipation at the same time.
For a full guide on recognizing inadequate intake, see: Signs You Are Not Eating Enough on GLP-1.
Cause 3: Low Fiber Intake
Dietary fiber plays a central role in digestive health. It adds bulk to stool, retains water, and helps move waste through the intestines efficiently. Without adequate fiber, stool becomes small, compact, and difficult to pass.
There are two types of fiber, and both matter:
- Soluble fiber dissolves in water and forms a gel-like substance that softens stool. It is found in oats, beans, and fruits like apples and pears.
- Insoluble fiber does not dissolve in water. It adds bulk and helps push waste through the colon faster. It is found in vegetables, whole grains, and seeds.
When people on GLP-1 medications eat significantly less food, they often unintentionally consume very little fiber. If the smaller meals they do eat are focused on protein without including enough vegetables, fruits, or whole grains, fiber intake can fall well below the recommended 25 to 38 grams per day for adults.
Fiber-rich foods to prioritize include: leafy greens, broccoli, berries, apples, oats, chia seeds, flaxseed, lentils, and chickpeas. These foods support healthy digestion and should be incorporated into every structured meal plan.
Fiber plays a central role in keeping digestion regular, but it becomes even more important when food intake is reduced. As explained by Harvard Health, the benefits of fiber for digestion include improving stool consistency, increasing bulk, and supporting healthy gut function — all of which are critical when dealing with slowed digestion on GLP-1.
Cause 4: Dehydration
Reduced appetite from GLP-1 medications does not just affect food intake — it can also suppress thirst signals. Many GLP-1 users report that they simply forget to drink enough water because they do not feel hungry or thirsty throughout the day.
Hydration is essential for healthy bowel movements. Water helps soften stool and keeps the digestive tract lubricated. When fluid intake is too low, the colon pulls extra water from waste material to compensate — the result is harder, drier stool that is much more difficult to pass.
Most adults need at least 8 to 10 cups of water per day under normal circumstances. GLP-1 users who are losing weight may have higher needs. Fluid intake should be consistent throughout the day rather than consumed in large amounts at once.
Cause 5: Electrolyte Imbalance
Electrolytes — including sodium, magnesium, and potassium — play a critical role in regulating muscle contractions throughout the body. This includes the smooth muscle contractions of the intestinal wall that push food and waste forward through the digestive tract.
When electrolyte levels drop, these contractions can become weaker and less frequent. The result is sluggish intestinal movement, which contributes directly to constipation. Magnesium is particularly important here — low magnesium is well-established as a contributor to constipation and is commonly addressed with both dietary changes and supplementation.
People on GLP-1 medications who are eating much less food may not be consuming enough electrolyte-rich foods. Potassium is found in bananas, avocado, and sweet potatoes. Magnesium is found in leafy greens, pumpkin seeds, and dark chocolate. Adequate sodium from whole food sources also supports gut motility.
⚠️ Why Constipation Can Stall Weight Loss
Constipation isn’t just uncomfortable — it can quietly slow down your progress. When digestion becomes sluggish, your entire metabolic flow is affected, making weight loss feel harder than it should be.
• Slower digestion = less efficient food movement, which can impact how your body processes nutrients
• Bloating and water retention = misleading scale readings, making it look like nothing is changing
• Digestive discomfort = lower energy and reduced activity, which directly affects calorie burn
Over time, this creates a frustrating loop where progress feels stalled — even when you’re doing everything right.
If this sounds familiar, it’s often connected to deeper metabolic factors. You can understand how your baseline metabolism plays a role here: Basal Metabolic Rate.
And if your weight loss has completely stalled despite eating less, read this breakdown: Why Am I Not Losing Weight on Ozempic — it explains the bigger picture behind these plateaus.
How to Relieve Constipation on GLP-1
Addressing GLP-1 constipation requires a consistent, multi-pronged approach. Drastic changes — like suddenly loading up on fiber or laxatives — can backfire and cause bloating, cramping, or diarrhea. Instead, focus on gradual, sustainable adjustments.
Increase fiber gradually
Add fiber slowly over one to two weeks rather than all at once. Start by adding one serving of vegetables or a high-fiber food to each meal. Rapid fiber increases can cause gas and bloating, especially on an already sensitive GLP-1 digestive system.
Prioritize consistent hydration
Set a reminder to drink water regularly throughout the day. Do not wait until you feel thirsty. A simple target is to consume at least 64 to 80 ounces of water daily, and more if you are physically active.
Eat balanced, structured meals
Avoid skipping meals entirely. Even if appetite is low, eating small, structured meals consistently helps stimulate digestive contractions. Include protein, vegetables, and a source of healthy fat at each meal.
Support electrolyte intake
Include foods rich in magnesium, potassium, and sodium. If dietary intake is consistently low, a magnesium supplement (like magnesium citrate or glycinate) may be worth discussing with a healthcare provider.
Move your body daily
Physical movement stimulates the digestive system. Even a 15 to 20 minute walk after meals can meaningfully improve gut motility and reduce constipation. This does not require an intense workout — consistent, moderate movement is what matters.
Maintain consistent meal timing
Eating at consistent times each day helps regulate the body’s natural digestive rhythm. Irregular eating patterns can further disrupt already slowed GLP-1 digestion.
Best Foods to Support Digestion on GLP-1
When eating smaller amounts of food, every meal needs to work harder nutritionally. These foods are especially effective at supporting digestive health during GLP-1 therapy:
- Non-starchy vegetables (spinach, kale, broccoli, zucchini) — provide insoluble fiber and water content.
- Berries (blueberries, raspberries, strawberries) — high in soluble fiber and antioxidants.
- Oats — a rich source of soluble fiber (beta-glucan) that softens stool and feeds gut bacteria.
- Chia seeds — absorb water and form a gel that adds bulk and moisture to stool.
- Plain yogurt with active cultures — supports gut bacteria diversity and intestinal function.
- Legumes (lentils, chickpeas, black beans) — excellent sources of both soluble and insoluble fiber, plus plant protein.
These foods do double duty — they support digestion while also contributing to nutrient density in smaller meal portions. When appetite is suppressed, choosing foods that deliver real nutritional value becomes more important than ever.
Protein Intake and Digestive Health
Adequate protein intake is a cornerstone of GLP-1 nutrition. During weight loss, the body is at risk of breaking down muscle tissue for energy — especially when food intake drops significantly. Prioritizing protein helps preserve lean muscle mass and supports metabolic function throughout the weight loss process.
From a digestive standpoint, protein should be combined thoughtfully with fiber and fluids. A high-protein diet without adequate fiber and hydration can worsen constipation. The goal is balance — not protein alone, but protein alongside the digestive support that fiber and water provide.
For a detailed guide on protecting muscle during GLP-1 therapy, see: Prevent Muscle Loss on GLP-1. For protein targets and strategies, see: How Much Protein on GLP-1 and How Much Protein Do You Really Need.
When Constipation May Require Medical Advice
Most cases of constipation on GLP-1 medications can be managed with the nutrition and lifestyle strategies outlined in this article. However, certain symptoms require prompt medical evaluation rather than self-management.
Contact your healthcare provider if you experience:
- Severe or persistent abdominal pain
- Constipation lasting longer than two weeks despite dietary changes
- Vomiting or persistent nausea alongside constipation
- Complete inability to pass stool for several days
- Blood in stool or unexplained rectal bleeding
These symptoms may indicate a more serious issue unrelated to GLP-1 medications and should always be evaluated by a qualified healthcare professional. This article is educational in nature and is not a substitute for medical advice.
A Structured Nutrition Strategy to Prevent GLP-1 Digestive Problems
Managing GLP-1 digestive side effects is not just about reacting to constipation when it appears. The most effective approach is building a nutrition structure that prevents digestive problems from becoming a recurring issue in the first place.
A structured metabolic nutrition strategy during GLP-1 therapy should include:
- Protein-first meals structured around daily intake goals
- Consistent fiber from vegetables, legumes, and whole foods at every meal
- Adequate daily hydration — at minimum 64 to 80 ounces of water
- Regular meal timing to support gut rhythm and stimulate digestion
- Daily movement to support gut motility and muscle preservation
The Fueled Framework system is built around exactly this kind of structured approach to metabolic nutrition during GLP-1 therapy. Rather than guessing about what to eat, Fueled Framework provides a clear, repeatable system that prioritizes muscle protection, energy stability, and digestive health simultaneously.
For a full meal planning framework designed specifically for GLP-1 users, see the: GLP-1 Meal Plan and Muscle Protection Guide.
If you’re dealing with constipation on GLP-1 medications, it’s rarely just a single issue — it’s part of a bigger metabolic picture. From hydration and fiber to protein intake and digestion speed, everything is connected. To understand the full system and how to optimize your results long term, explore the complete guide here: GLP-1 Nutrition Guide — your central resource for building a sustainable strategy while using Ozempic, Wegovy, or Mounjaro.
Frequently Asked Questions About GLP-1 Constipation
Why does GLP-1 cause constipation?
GLP-1 medications slow gastric emptying and reduce the rate at which the digestive system moves food through the intestines. This slowed motility, combined with reduced food intake and often lower fiber and fluid consumption, creates the conditions for constipation. For more info on constipation causes and treatment check out Cleaveland Clinic
Does constipation go away on GLP-1?
For many people, constipation improves as the body adjusts to the medication — usually within the first few weeks to months. However, improvement is more reliable when nutrition strategies are actively in place. Without attention to fiber, hydration, and meal structure, constipation can persist throughout GLP-1 therapy.
How long does GLP-1 constipation last?
The timeline varies by individual. Some people experience constipation only during the early weeks of starting or increasing their GLP-1 dose. Others find it is an ongoing issue throughout treatment, particularly if dietary fiber and hydration are not adequately addressed. Consistent nutrition habits can shorten the duration significantly.
What foods help constipation on GLP-1?
Foods highest in fiber and water content are most helpful. Prioritize vegetables like broccoli and leafy greens, fruits like berries and pears, chia seeds, oats, lentils, and chickpeas. Pairing these with consistent water intake makes them significantly more effective for relieving constipation.
Should I take fiber supplements on GLP-1?
Fiber supplements such as psyllium husk can be helpful when dietary fiber intake is consistently low. However, they should be introduced gradually and taken with plenty of water. Supplements are not a replacement for whole food fiber sources, which deliver additional nutrients and gut-health benefits alongside fiber.
Conclusion
GLP-1 constipation is a common and understandable side effect of how these medications work. Slowed digestion, reduced food intake, lower fiber consumption, dehydration, and electrolyte imbalance all play a role — and in most cases, all of them need to be addressed together.
The encouraging reality is that GLP-1 digestive side effects are manageable. Most people experience meaningful improvement when they adopt structured nutrition habits that prioritize fiber, hydration, balanced meals, and consistent meal timing. These are not complicated changes — but they do need to be intentional.
If you are on a GLP-1 medication and struggling with constipation, start with the basics: increase fiber gradually, drink more water consistently, avoid skipping meals entirely, and add daily movement to your routine. Small, consistent adjustments compound over time.
A structured metabolic nutrition strategy — like the one Fueled Framework is built around — gives GLP-1 users a clear system for managing these challenges while still progressing toward their health and body composition goals. Nutrition clarity removes the guesswork and makes the process more sustainable from the start.